HIV and mobility in Australia: road map for action
HIV and mobility in Australia: road map for action
HIV Australia | Vol. 13 No. 1 | March 2015
By Gemma Crawford,1 Roanna Lobo2 and Graham Brown3
HIV epidemics throughout their history have been influenced by international mobility, changing as a result of globalisation, rapid urbanisation and mass mobility. In the last decade, the issue has been growing in profile in Australia due to increasing HIV diagnoses related to international mobility.
Australia has been one of a number of high income countries experiencing a disproportionate number of new HIV diagnoses among people from high prevalence regions, particularly from sub Saharan Africa and South East Asia.
While the majority of HIV diagnoses in Australia are among Australian residents, and primarily amongst gay men, in some jurisdictions such as Western Australia, HIV among internationally mobile communities comprises more than 50% of new diagnoses.
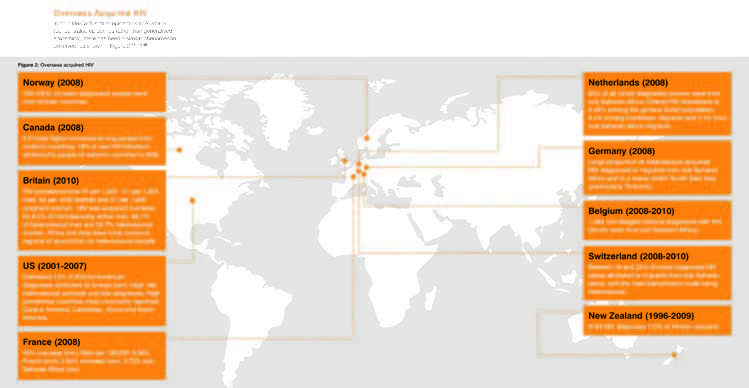
Similar diversifying epidemics related to increased mobility between high and low prevalence countries have been identified across North America and Europe (see Figure 1 – click on image for larger version).
Australia has used a combination of strategies to respond to HIV with a focus on prevention. These include:
- mobilising communities most impacted by HIV
- encouraging individuals in priority groups to reduce risk behaviour, undergo regular HIV testing and start and maintain treatment
- changing government laws and modifying policies to ensure that a human rights approach underpinned the Australian HIV response and that other strategies could be implemented, and
- undertaking appropriate surveillance, research and evaluation to guide and inform responses.
However, the relationship between HIV and mobility is complex and the causal links between HIV and the experiences of people travelling to and from regions of high HIV prevalence are not well understood. Overlayed are issues of stigma, racism and marginalisation as well as historical contexts such as colonisation, evolving economic and migration policies, and labour mobility.
These complexities have resulted in an emphasis on short-term, small-scale projects and research studies, both in Australia and elsewhere.
The Seventh National HIV Strategy 2014–20171 identifies people from high prevalence countries and their partners, and travellers and mobile workers as priority populations (see Figure 2), but provides little guidance as to priority action. (Click on image for large version.)
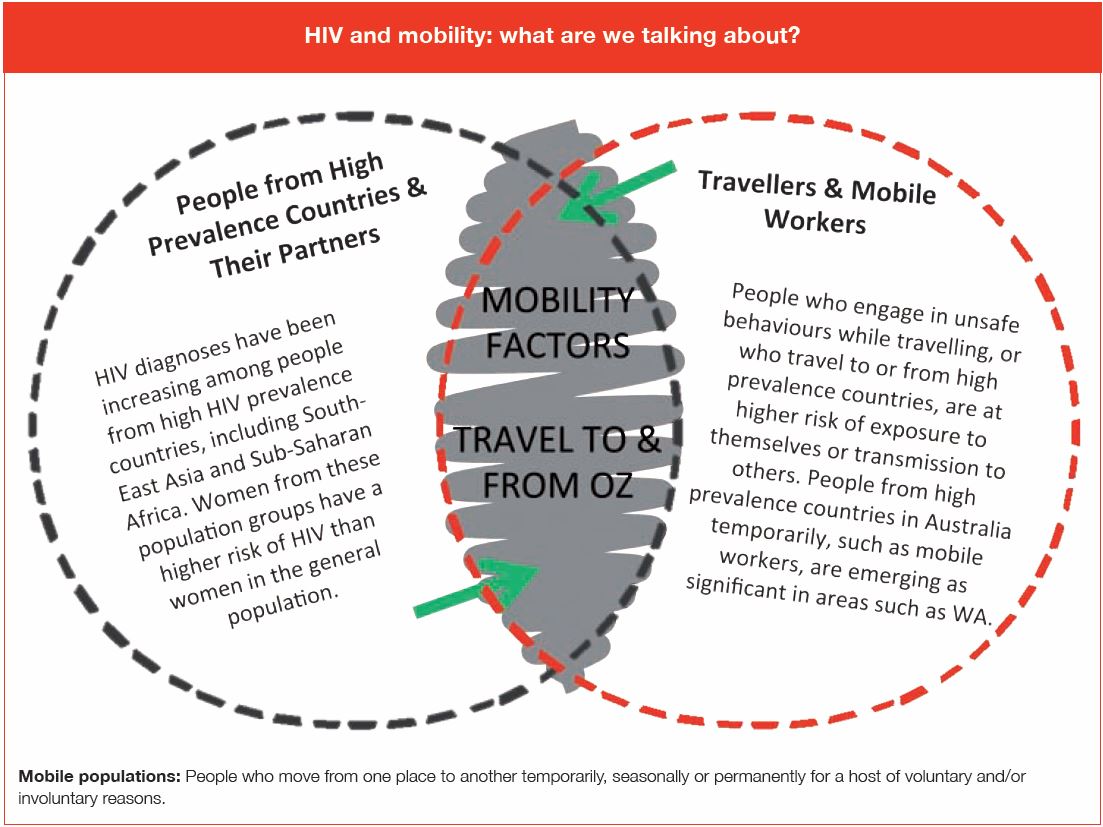
Much of Australia’s policy response to HIV and mobility has been relegated to the ‘needs attention’ category but with no harmonised policy and program response. Without an integrated response across government, community, health services and research there will be little progress in this emerging priority for the Australian HIV epidemic.
The HIV and Mobility in Australia: Road Map for Action2 has been developed to move the discussion from rhetoric to comprehensive and coordinated action.
The Road Map is an outcome of a partnership between the Collaboration for Evidence, Research and Impact in Public Health (CERIPH) (formerly the Western Australian Centre for Health Promotion Research) and the Australian Research Centre in Sex, Health and Society (ARCSHS), with support from the Sexual Health and Blood-borne Virus Applied Research and Evaluation Network (SiREN) and funding from the Commonwealth Department of Health.
The Road Map proposes a way forward for the Australian HIV partnership and is informed by:
- the Seventh National HIV Strategy 2014–2017
- frameworks and approaches successfully used in Australia
- frameworks and approaches used with mobile populations and migrants in similar countries
- relevant research from Australia and overseas, and
- consultation with key community, policy and research stakeholders.
The Road Map outlines ten principles and over 70 strategies across five action areas to support a strategic approach to HIV management for mobile populations and migrants in Australia (see breakout boxes: ‘Ten principles for a strategic approach to HIV and mobility’ and ‘Five areas for action’, below.)
Next steps
HIV has always been, and still is, a condition related to population movement and mobility. Despite this, many governments and regions have been slow to understand the impact of mobility on local HIV epidemics and local responses.
Read the HIV and Mobility: Road Map for Action report (siren.org.au/hivandmobility or www.latrobe.edu.au/arcshs/publications), share it with others, talk about it.
Join the Coalition for HIV and Mobility Issues to progress action on advocacy, research, policy and practice. Please email expressions of interest to SiREN at siren@curtin.edu.au
Get involved in discussion via Twitter #HIVMobile.
Look for opportunities to partner with others to explore the issues.
Keep HIV and Mobility on the agenda.
However, some governments and regions have developed strategies and approaches in response to the increase in HIV infections related to mobile populations that are starting to pay dividends.
The Road Map has drawn on these experiences, and the work to date in Australia, and applied them to the emerging Australian context.
The Road Map is intended to generate discussion and action among key stakeholders including community organisations, health services, research institutions, government bodies and policy makers and provides a way forward to respond to these emerging challenges with courage, creativity and commitment.
Subsequent to the launch of the Road Map on World AIDS Day 2014, the Western Australian Department of Health has provided funds to support a Coalition for HIV and Mobility Issues.
The coalition will comprise policy, community, health service and research members to progress action towards the recommendations of the Road Map (contact siren@curtin.edu.au for further details).
This work would not have been possible without input from a number of people. Thanks to those who provided direct input in to the report. Thanks also to authors Trish Langdon, Gemma Crawford, Roanna Lobo, and Graham Brown.
Ten principles for a strategic approach to HIV and mobility
- Incorporate a human rights approach – stigma and discrimination directed at mobile populations and migrants must be reduced
- Reduce all barriers to testing and access to treatment
- Pay attention to the confluence between HIV and mobility
- Move beyond ‘narrow protectionist policies’
- Commit resources to improve migrant health
- Continue to develop links and cooperative partnerships with affected communities locally and internationally
- Participate in and contribute to global health governance
- Create closer cooperation between Australia and the HIV policy, public health, treatment and support sectors in countries of origin and destination for Australian mobile populations and migrants
- Acknowledge that mobile population and migrants need more than information (even if it is translated). Specialist services as well as generalised services need to be provided
- Know your epidemic(s) – continue surveillance and monitoring and develop evaluation strategies in conjunction with migrant populations.
Five areas for action
The Road Map identifies over 70 strategies with proposed primary responsibilities and suggested timeframes. Some key themes are highlighted below.
- International Leadership and Global Health GovernanceFor example – Australia is well placed to participate in and contribute to international dialogue on cross border HIV responses, providing policy leadership to minimise rates of HIV as a result of mobility in the Pacific region and to ensure that Australia’s own policies are consistent with this outcome
- Commonwealth and State leadershipFor example – ensuring the Australian HIV response enables an effective response to migrants and mobile populations that experience increased vulnerability to HIV acquisition or transmission, within a human rights framework. This includes providing strong leadership in relation to building overall community support and consensus to prioritisation of health services related to mobile populations and migrants and coherent legal and policy responses to mobile populations and migration.
- Community mobilisationFor example – supporting partnerships between migrant groups, other community groups and the HIV sector to advocate for change and improvements in health and other service delivery; encouraging leadership and peer advocacy within migrant and mobile populations and increase participation in the HIV response; and improving mobile population and migrant community awareness, health literacy, knowledge, attitudes and risk reduction behaviours around HIV in the context of living in Australia
- Development of services for mobile or migrant people and groupsFor example – increase the uptake of sexual health testing, treatment, education and referral amongst migrants and mobile populations with an emphasis on early detection and treatment and supporting the health and wellbeing of migrants and other mobile people living with HIV. This will require improved understanding of the cultural and structural impacts of services on mobile populations and migrants, decreased discriminative attitudes towards migrants and other mobile people with HIV, and increased health literacy of migrants and mobile population.
- Surveillance, research and evaluationFor example – invest in high quality research to inform the strategic and policy response to mobile populations and migrants such as: standardised surveillance for sub populations; evaluation of interventions for migrants and mobile populations, including universal access to treatment; social research on migrant healthcare seeking behaviours, HIV knowledge and attitudes, and experiences of migrants living with HIV; analysis of barriers to uptake, maintenance and effectiveness of treatment; role and feasibility of treatment as prevention in migrant populations; and investigation of impacts of legislation on migrant health and access to HIV treatment.
References
1 Australian Government Department of Health. (2014). Seventh National HIV Strategy 2014–2017. Commonwealth of Australia, Canberra.
2 Crawford, G., Lobo, R., Brown, G., Langdon, P. (2014). HIV and mobility in Australia: Road map for action. Western Australian Centre for Health Promotion Research, Perth, Australian Research Centre in Sex, Health and Society, Melbourne.
Author references
1 Collaboration for Evidence, Research and Impact in Public Health (CERIPH), Curtin University
2 Sexual Health and Blood-borne Virus Applied Research and Evaluation Network (SiREN), Curtin University
3 Australian Research Centre in Sex, Health and Society (ARCSHS), La Trobe University

